The Classic Comprehensive Handbook of Cat Care: PROTOZOANS
There are few intestinal protozoans that cause illness in cats. Signs of infection, if present, are variable but often include diarrhea not responsive to home treatment. There is no method to diagnose or treat these parasites at home, so you as an owner must rely on the help of a veterinarian, who can diagnose their presence microscopically or with special lab tests and prescribe proper medication.
The most common intestinal protozoal infections of cats are by coccidia o r Giardia organisms, and most are self-limiting and asymptomatic. However, kittens that are raised in dirty environments highly contaminated by parasites may become ill and develop diarrhea (sometimes bloody) when infected with coccidia or Giardia.
TOXOPLASMA INFECTION
One coccidia of special interest is Toxoplasma gondii. This microscopic organism is found in all parts of the world. Like other members of its class it is able to produce signs of intestinal disease (e.g., diarrhea) in cats, but it also has a tissue phase that can produce serious generalized disease. At times it can become a human health hazard.
HOW TOXOPLASMA IS ACQUIRED
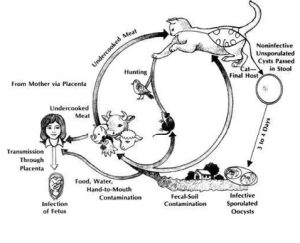
Cats and other mammals, including humans, may acquire Toxoplasma before birth when the mother becomes newly infected during pregnancy or when a previously acquired but quiescent infection becomes reactivated. The more likely sources of infection for a pet cat are the consumption of undercooked or raw meat (including wild caught rodents or birds) containing the infective tissue stages of the disease. These oocysts can contaminate soil where they can be picked up by the feet or fur of a passing cat or other mammal and later ingested while grooming. Infected soil can contaminate food products such as milk or vegetables, and oocysts can be transported by flies and cockroaches from contaminated soil or oocyst-infected cat stool to surfaces where they may be accidentally ingested.
TOXOPLASMA LIFE CYCLE
After infection, signs of disease may or may not be seen depending on many factors including age, the presence of concurrent infections (e.g., feline leukemia virus, feline immunodeficiency virus) and general state of health. In general, signs of illness are most likely to develop in kittens, very old cats, or others who have weakened immune systems. If signs do develop, they may be as simple as diarrhea or so complex as to mimic many other diseases. Signs that have been seen include fever, lack of appetite, lethargy, enlarged lymph nodes, weight loss, coughing and difficulty breathing, signs of pancreas and/or bowel inflammation (e.g., vomiting, diarrhea), signs of liver disease including vomiting and yellowish gums, and eye or nervous system problems. Nervous system signs can result in almost any disorder including personality changes, seizures, loss of bowel and/or bladder control to difficulty walking or even heightened sensitivity to touch. Pregnant cats may abort. Because of the many possibilities involved, diagnosis must be made with the help of a veterinarian who will use laboratory tests to confirm the infection.
TOXOPLASMA INFECTION IN HUMANS IS NOT USUALLY SERIOUS
Alarmist articles concerning toxoplasmosis in people and in cats have appeared in newspapers and popular magazines. They have often emphasized the congenital type of transmission from pregnant women to their unborn children, which can result in severe birth defects and infant death, and they have often dwelt on the possibility of acquiring infection from cat stool. In fact, birth defects due to Toxoplasma infection are relatively rare, and the disease in healthy adult humans is commonly so mild that it passes undiagnosed. Research indicates that 30 to 60% of adults in the United States have had toxoplasmosis; in other countries the incidence is much higher. It is now known that toxoplasmosis in humans is a common infection but a rare cause of disease. (The exception is the individual with a weakened immune system such as the AIDS patient or transplant recipient.) Although human infection can be acquired from material contaminated with infected cat feces, adults are more likely to contract toxoplasmosis from eating raw or undercooked meat than by contact with cats. (Infection rates of more than 80% have been found in people who eat raw meat, especially those eating undercooked lamb and pork.) Children, on the other hand, are most likely to become infected by coming into contact with soil that has been contaminated with cat feces containing Toxoplasma. This is because children are more likely to put contaminated soil or other dirty objects in their mouths, and they are much less likely than adults to wash their hands and fingernails after playing in the dirt.
Since cats (both wild and domestic) are the only animals that shed the infective stages of Toxoplasma in their stools, it is important to control toxoplasmosis in cats to break the cycle of transmission to other animals and to people.
TOXOPLASMOSIS PREVENTION
Toxoplasmosis can be easily prevented in your cat by observing the folowing rules:
- Feed only pasteurized dairy products, commercial cat foods that have been subjected to heat during processing, or thoroughly cooked meat (heat through to 140°F, [60°C]). (Meat frozen to temperatures below – 68°F (—20°C) and thawed before feeding is safe, but most home freezers cannot meet these requirements, and it is, therefore, unsafe to feed any uncooked meat to your cat.)
- Confine your cat to prevent capture and consumption of Toxoplasma- infected birds or rodents and to prevent contact with the feces of infected carrier animals. Bell cats who cannot be confined indoors to limit any successful hunting.
Blood tests are available through physicians for individuals who would like to find out whether they have been previously infected by Toxoplasma and are, therefore, immune to further infection. Human infections can be minimized by strictly following the recommendations listed below. Pregnant women or women contemplating pregnancy who have not been previously infected with toxoplasma should be particularly careful to follow these guidelines.
- Avoid eating unpasteurized dairy products or raw or undercooked meat of any type (heat through to 140°F, [60°C]). Wash your hands after handling raw meat.
- Take cats showing signs of illness to be examined by a veterinarian who can perform a fecal examination for Toxoplasma organisms. Cats shedding oocysts should be hospitalized or isolated in some other manner until the shedding stops (in about ten to fourteen days) to prevent further transmission of the organism.
- Follow the rules for preventing Toxoplasma infection of cats.
- Avoid careless handling of stools of cats that are allowed to contact sources of Toxoplasma infection. In rural areas, cats should not be allowed to defecate in hay racks, feeding troughs, or other areas where farm animals may eat. Provide litter boxes for them which will encourage defecation in relatively controlled sites. Remove stool from the litter box daily (organisms in stool take two to four days at average room temperatures to become infective), and use disposable pan liners or disposable cat boxes if possible. Nondisposable cat litter pans should be scalded with water heated to 131°F, (50°C) or disinfected with 10% ammonia solution whenever the litter is replaced. Dispose of cat litter and stool by flushing it down the toilet or burning it. Wear disposable gloves while cleaning the litter pan.
- Wear gloves while gardening to prevent contact with Toxoplasma- contaminated soil.
- Cover children’s sandboxes when not in use to prevent fecal contamination.
- Control cockroaches, flies, rodents, and stray cats, which can act as transport hosts and carriers of the Toxoplasma organism.
- Avoid handling or holding free-roaming cats close to your mouth in order to prevent contact with feet or fur that could have touched infected soil. Keep free-roaming cats off bedding, tables, and counter tops.
- Wash all uncooked, possibly soil-contaminated vegetables thoroughly before eating.
- Make thorough handwashing and nail scrubbing a part of each child’s and adult’s daily routine, especially following contact with free- roaming cats, farm animals, soil, unpasteurized dairy products, and uncooked meat or vegetables.